What Is Psilocybin? The Science, Therapeutic Research, and Legal Landscape
March 13, 2026 2026-03-13 13:40What Is Psilocybin? The Science, Therapeutic Research, and Legal Landscape
What Is Psilocybin? The Science, Therapeutic Research, and Legal Landscape
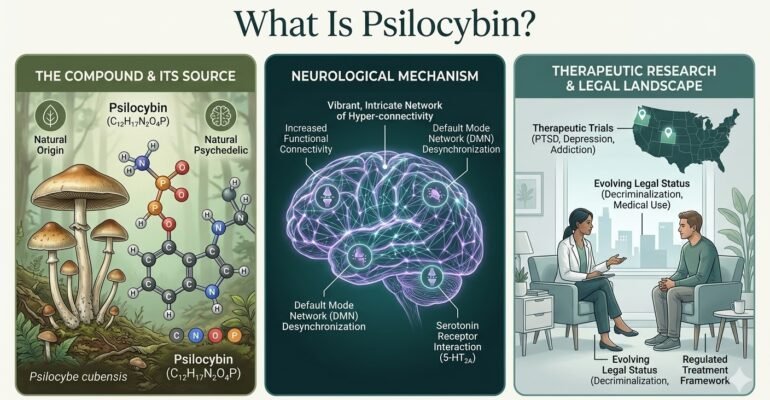
What Is Psilocybin? The Science, Therapeutic Research, and Legal Landscape
Once dismissed as a dangerous hallucinogen with no medical value, psilocybin is now one of the most actively researched compounds in psychiatry. With FDA Breakthrough Therapy designations, landmark trials from Johns Hopkins and NYU, and shifting state laws across the US, psilocybin sits at a remarkable crossroads of ancient human history and cutting-edge neuroscience. This guide explains what it is, what the science actually shows, and what the evolving legal landscape means for patients.
In this article
- What is psilocybin? Chemistry and origins
- How psilocybin works in the brain
- What the psilocybin experience involves
- Therapeutic research: conditions under study
- How psilocybin-assisted therapy works
- Safety profile and risks
- Psilocybin vs. other psychedelics
- Legal status: US and global landscape
- Frequently asked questions
What is psilocybin? Chemistry and origins
Psilocybin is a naturally occurring psychedelic compound found in over 200 species of fungi — commonly referred to as “magic mushrooms” or “shrooms.” Chemically, it is a tryptamine compound (4-phosphoryloxy-N,N-dimethyltryptamine) that the body rapidly converts into its active form, psilocin, after ingestion.
Psilocin is structurally similar to serotonin, the brain’s primary mood-regulating neurotransmitter — a resemblance that directly explains its profound effects on perception, emotion, and cognition.
Psilocybin-containing mushrooms have been used by indigenous cultures in Mesoamerica for thousands of years in ceremonial and spiritual contexts. The Mazatec people of Oaxaca, Mexico, referred to them as “teonanácatl” — flesh of the gods. Their ritual use was documented by Spanish colonizers in the 16th century and effectively suppressed for centuries.
Modern scientific interest began in 1958 when Swiss chemist Albert Hofmann (who had earlier synthesized LSD) isolated and identified psilocybin and psilocin from the mushroom species Psilocybe mexicana. Harvard psychologist Timothy Leary conducted some of the first clinical studies in the early 1960s, before psilocybin was swept up in the broader criminalization of psychedelics under the Controlled Substances Act of 1970.
How psilocybin works in the brain
Psilocybin’s primary mechanism of action is as a partial agonist at serotonin 2A (5-HT2A) receptors — the same receptors targeted by classical psychedelics like LSD and DMT. This is distinct from MDMA’s mechanism and explains why psilocybin produces genuinely perceptual and consciousness-altering effects rather than primarily emotional ones.
Default mode network disruption
One of the most important neuroscientific findings in psilocybin research involves the default mode network (DMN) — a set of interconnected brain regions associated with self-referential thinking, rumination, the sense of a fixed “self,” and the maintenance of habitual thought patterns. In depression, the DMN is often hyperactive and rigidly organized.
Neuroimaging studies show that psilocybin dramatically reduces activity in the DMN and temporarily disrupts its rigid connectivity — an effect researchers describe as “entropic brain activity.” This loosening of fixed neural patterns is hypothesized to create a window of neuroplasticity during which new, healthier thought patterns can take root — particularly when supported by psychotherapy.
Neuroplasticity and synaptogenesis
Beyond the DMN, preclinical research (primarily in rodents) has shown that psilocybin promotes the growth of new dendritic spines — the structural connections between neurons — at remarkably low doses. This structural neuroplasticity may underlie the lasting antidepressant effects observed in clinical trials, where patients report improvements persisting for months after just one or two doses.
A 2021 study published in Neuron found that a single dose of psilocybin increased dendritic spine density in the mouse prefrontal cortex by approximately 10%, with structural changes persisting for at least a month. This provides a potential biological mechanism for psilocybin’s durable therapeutic effects.
Increased neural cross-talk
Psilocybin also enables communication between brain regions that do not normally interact — a phenomenon sometimes visualized as a “hyperconnected” brain state. This may explain the synesthetic, perspective-shifting, and insight-generating qualities of the psilocybin experience, and is thought to support the creative cognitive reorganization that underlies therapeutic benefit.
What the psilocybin experience involves
The psilocybin experience — sometimes called a “journey” or “trip” in both clinical and lay contexts — varies significantly by dose, setting, individual psychology, and intention. In clinical trials, carefully controlled conditions are used to maximize therapeutic value and minimize distress.
Perceptual effects
- Visual patterns, enhancement of colors
- Altered perception of time and space
- Synesthesia (blending of senses)
- Visual hallucinations at higher doses
- Heightened sensory sensitivity
Psychological effects
- Deep introspection and self-reflection
- Emotional release and catharsis
- Sense of interconnectedness
- Mystical or transcendent experiences
- Dissolution of ego boundaries
- Confrontation of suppressed emotions
Duration and timeline
Psilocybin typically takes effect within 20–60 minutes of ingestion, reaches peak intensity around 2–3 hours, and resolves over 4–6 hours total. This profile makes it more manageable for clinical settings than LSD, which can last 8–12 hours.
Challenging experiences (“difficult trips”)
Not all psilocybin experiences are pleasant. Anxiety, confusion, paranoia, and overwhelming emotions can occur — particularly at higher doses or in unsupportive environments. In clinical research, these challenging experiences are considered a potential part of the therapeutic process when properly supported, but they underscore why set (mindset), setting (environment), and skilled therapeutic guidance are considered essential in any clinical application.
Therapeutic research: conditions under study
Psilocybin has received considerable research attention across a growing range of psychiatric and neurological conditions. Here is where the science currently stands:
Treatment-resistant depression and major depressive disorder
This is the most advanced area of psilocybin research. Psilocybin has received two FDA Breakthrough Therapy designations — one for treatment-resistant depression (2018) and one for major depressive disorder (2019) — based on early trial results suggesting substantial improvement over existing treatments.
A landmark 2021 trial at Imperial College London compared psilocybin therapy directly to the SSRI escitalopram (Lexapro) over 6 weeks. Psilocybin was comparable on the primary outcome measure, but showed advantages on several secondary measures including emotional well-being and functioning — and with only two doses rather than daily medication.
End-of-life anxiety and existential distress
Some of the most compelling early research involved patients with life-threatening cancer experiencing anxiety, depression, and existential distress. Trials at Johns Hopkins and NYU found that a single high dose of psilocybin produced rapid, substantial, and durable reductions in depression and anxiety — with 60–80% of participants showing clinically significant improvements at 6-month follow-up. Many participants described the experience as among the most meaningful of their lives.
Other conditions under active investigation
- Alcohol use disorder — early trials show promising reductions in heavy drinking days
- Tobacco addiction — a Johns Hopkins pilot study showed 80% abstinence rates at 6 months, far exceeding standard treatments
- Obsessive-compulsive disorder (OCD)
- Anorexia nervosa
- PTSD (often studied alongside MDMA research)
- Migraine and cluster headaches
- Alzheimer’s disease (early-stage investigation)
How psilocybin-assisted therapy works
Like MDMA-assisted therapy, psilocybin therapy is never just medication — it is a structured combination of psychotherapy and carefully administered drug sessions. The drug is considered a catalyst or amplifier for the therapeutic process, not a standalone treatment.
Preparation (2–3 sessions): Therapists build a strong therapeutic alliance with the patient, explore their history and intentions, and explain what to expect. This groundwork is considered essential for a safe and productive experience.
Psilocybin session (1–2 sessions): The patient receives a single carefully measured dose in a comfortable, carefully designed clinical room. They lie on a couch wearing eyeshades and headphones with curated music, while two trained therapists remain present throughout the 5–6 hour session, offering support without directing the experience.
Integration (2–4 sessions): Therapy sessions in the days and weeks following each psilocybin session help the patient process insights, emotions, and realizations that emerged — translating them into lasting behavioral and psychological change.
Researchers consistently emphasize that the quality of the therapeutic relationship, the setting, and post-session integration work are as important as the drug itself. Psilocybin without this structured support framework does not produce the same clinical outcomes.
Safety profile and risks
Psilocybin has one of the most favorable safety profiles of any psychoactive substance studied in clinical research. It is non-toxic, non-addictive, and carries no known lethal dose in humans. However, this does not mean it is without risk — context matters enormously.
Physical safety
Psilocybin produces modest cardiovascular effects — mild increases in heart rate and blood pressure — but does not cause organ toxicity. It does not suppress respiration like opioids or cause dangerous hyperthermia like MDMA. There are no documented human fatalities directly attributable to psilocybin toxicity.
Psychological risks
- Acute anxiety, panic, or overwhelming emotional experiences — manageable with proper support
- Transient psychosis-like states at very high doses
- Triggering of latent psychiatric conditions in vulnerable individuals — particularly those with a personal or family history of schizophrenia or bipolar I disorder
- Hallucinogen Persisting Perception Disorder (HPPD) — a rare condition where visual disturbances persist after the drug has worn off
Important contraindications: Psilocybin is not appropriate for individuals with a personal or family history of schizophrenia, schizoaffective disorder, or bipolar I disorder, due to the risk of precipitating or worsening psychosis. Rigorous participant screening is a core component of all clinical trial protocols for this reason.
Addiction potential
Psilocybin does not activate the dopamine reward pathway in the way that addictive substances do. It does not cause physical dependence or withdrawal. In fact, as noted in the addiction research above, it is being studied as a treatment for addictive disorders. The WHO’s Expert Committee on Drug Dependence has repeatedly assessed psilocybin mushrooms as having low abuse potential.
Psilocybin vs. other psychedelics
Psilocybin
Natural (fungal), 4–6 hr duration, serotonin 2A agonist, low toxicity, FDA Breakthrough designation, in Phase 3 trials
LSD
Synthetic, 8–12 hr duration, serotonin 2A agonist, similar mechanism to psilocybin, less clinical research, still Schedule I
MDMA
Synthetic, 3–5 hr duration, primarily serotonin/dopamine releaser, empathogen not classical psychedelic, Phase 3 PTSD trials
Ketamine
Synthetic, 45–60 min duration, NMDA antagonist, FDA-approved (esketamine), widely available in clinics now
DMT / Ayahuasca
Natural, short-acting alone (15–30 min), serotonin 2A agonist, early research for depression and addiction, no FDA designation yet
Ibogaine
Natural (plant), 18–36 hr duration, complex mechanism, studied for opioid addiction, cardiac risks, decriminalized in some jurisdictions
Legal status: US and global landscape
Psilocybin remains a Schedule I controlled substance under US federal law, meaning it is officially classified as having no accepted medical use and a high potential for abuse. However, the legal landscape is shifting rapidly at the state and city level — and internationally.
| Jurisdiction | Status | Details |
|---|---|---|
| US Federal | Schedule I | Illegal; FDA Breakthrough Therapy designation allows research |
| Oregon | Legal (regulated) | Measure 109 (2020) created licensed psilocybin service centers; programs active since 2023 |
| Colorado | Legal (regulated) | Proposition 122 (2022) legalized regulated “natural medicine” healing centers; rollout underway |
| Several US cities | Decriminalized | Denver, Oakland, Santa Cruz, Washington DC, Seattle, and others have deprioritized enforcement |
| Netherlands | Partial tolerance | Psilocybin mushrooms banned; psilocybin truffles legal and widely available in retreat settings |
| Jamaica | Legal | No prohibition on psilocybin; home to numerous legal retreat centers |
| UK | Class A | Most restrictive classification; significant criminal penalties |
| Australia | Approved (medical) | TGA reclassified psilocybin as Schedule 8 (controlled medicine) for treatment-resistant depression in 2023 — first country to do so |
Australia made history in 2023 by becoming the first country in the world to formally approve psilocybin as a prescription medicine for treatment-resistant depression, administered through authorized psychiatrists under strict protocols. This regulatory milestone is closely watched by regulators in other countries.
The path toward FDA approval in the US
Several companies — including Compass Pathways, USONA Institute, and Synthesis Institute — are conducting Phase 2 and Phase 3 trials working toward FDA approval. Compass Pathways’ synthetic psilocybin (COMP360) is furthest along in the regulatory process for treatment-resistant depression. If trials succeed, FDA approval could realistically arrive in the next 3–5 years, though timelines remain uncertain.
Frequently asked questions
Is psilocybin the same as magic mushrooms?
Psilocybin is the active compound found in magic mushrooms — but they are not the same thing. Magic mushrooms (primarily species in the Psilocybe genus) contain psilocybin along with other compounds including psilocin, baeocystin, and norbaeocystin. In clinical research, pharmaceutical-grade synthetic psilocybin is used for precise, consistent dosing. The effects are essentially the same, but controlled research requires standardized compounds.
Can psilocybin cause a “bad trip”?
Yes. Challenging psychological experiences — anxiety, paranoia, frightening visions, and overwhelming emotions — can occur, particularly at high doses or in unsupportive environments. In clinical settings, these are minimized through careful screening, preparation, a calming physical environment, and the continuous presence of trained therapists. Context — set and setting — is one of the most important determinants of psilocybin experience quality.
How is psilocybin different from antidepressants?
Traditional antidepressants like SSRIs require daily use and typically take 4–6 weeks to produce effects. Psilocybin therapy involves just one or two supervised sessions and has shown antidepressant effects that persist for weeks to months. Mechanistically, SSRIs modulate serotonin availability gradually; psilocybin produces acute, intense activation of serotonin receptors and promotes structural neuroplasticity. They work in fundamentally different ways — and some researchers believe they may eventually be used complementarily.
Can I access psilocybin therapy today?
In the US, legal access is currently limited. Oregon and Colorado have regulated service frameworks, and clinical trials are recruiting participants at several research institutions. Outside clinical trials or these state programs, psilocybin remains federally illegal. In Australia, authorized psychiatrists can now prescribe pharmaceutical psilocybin. In Jamaica and the Netherlands, legal retreat options exist. Always verify the legal status in your jurisdiction before pursuing any access.
Is psilocybin therapy covered by insurance?
Not currently in the US, as psilocybin lacks FDA approval for any indication. In Australia, where it is approved for treatment-resistant depression, insurance coverage varies by plan. As FDA approval progresses, insurance coverage will be a critical access issue — one that advocacy groups and researchers are actively raising with policymakers.
Will psilocybin make me lose control?
Many people worry about this. Psilocybin does not cause the same loss of motor control or behavior as alcohol or other substances. People remain physically coordinated and able to speak during sessions. However, the inner psychological experience can be deeply immersive and emotionally intense — which is why experienced therapeutic support is considered essential, and why sessions take place in a reclined, supported position.
Interested in learning more about psychedelic-assisted therapies or finding qualified practitioners? ThePsycheStore.com is building a trusted resource library to guide patients through emerging mental health treatments.
Medical and legal disclaimer: This article is for informational and educational purposes only. Psilocybin is a Schedule I controlled substance under US federal law and is illegal in most jurisdictions outside of licensed research or regulated state programs. Nothing in this article constitutes medical advice, encouragement to use psilocybin outside a legal framework, or guidance on obtaining controlled substances. If you are experiencing depression, PTSD, or another mental health condition, please consult a licensed healthcare professional about evidence-based treatment options available to you.
Search
Categories

